Mental Health Integration in Healthcare Systems in the USA
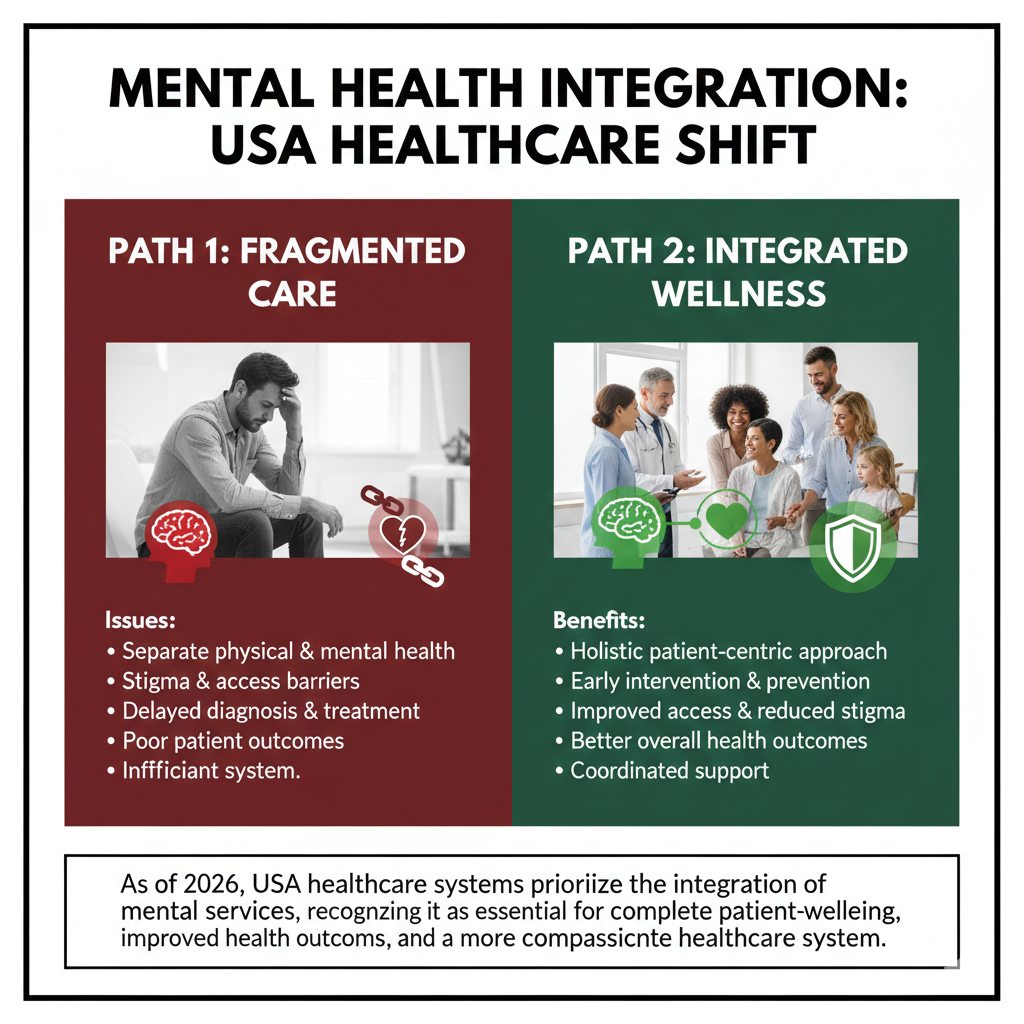
For generations, the American healthcare system has operated with a distinct line drawn down the center. On one side, you have physical health—broken bones, heart conditions, and the flu. On the other side, isolated and often stigmatized, sits mental health. You go to a primary care clinic for a cough, but you are often handed a referral slip and told to find a specialist across town if you mention anxiety.
This separation doesn’t reflect how human beings actually function. Our mental and physical health are deeply intertwined. Stress can cause high blood pressure, and chronic illness can trigger depression. Treating them separately often leads to fragmented care, missed diagnoses, and poorer health outcomes.
Fortunately, a shift is occurring across the United States. Healthcare systems are moving toward mental health integration, a model that treats the mind and body together. This approach promises to close the gap between physical and behavioral medicine, making it easier for patients to get the comprehensive care they need without jumping through administrative hoops.
What Is Mental Health Integration?
At its core, mental health integration is the systematic coordination of general medical care and behavioral healthcare. Instead of treating these two aspects of health in different buildings with different systems, integrated care brings them together.
In a traditional, non-integrated setting, a primary care physician might notice signs of depression in a patient but lack the resources to treat it immediately. The patient is referred out, and statistics show that many never follow through with that appointment due to confusion, cost, or fear.
In an integrated care model, behavioral health is woven into the fabric of primary care. A patient visiting for a routine physical might be screened for depression. If they need support, a behavioral health specialist might step into the room right then and there. It transforms mental health from a “specialist” issue into a standard part of staying healthy.
Why Mental Health Integration Matters in the USA
The United States is facing a mental health crisis. Rates of anxiety, depression, and substance use disorders have risen sharply over the last decade, yet the healthcare infrastructure has struggled to keep pace.
Millions of Americans live in areas designated as Mental Health Professional Shortage Areas. Even in cities with plenty of providers, navigating insurance networks and waitlists can be a nightmare. This creates a massive gap in access. People often wait until they are in crisis before seeking help, leading to expensive emergency room visits and severe suffering.
Integration matters because primary care is the “front door” of the healthcare system. Most people visit a general doctor at least once a year. By embedding mental health support in these visits, the system catches issues that would otherwise slip through the cracks. It ensures continuity of care, meaning your doctors are talking to each other and working off the same playbook.
Models of Mental Health Integration
Integration isn’t a one-size-fits-all solution. Different clinics and hospital systems adopt different frameworks depending on their resources and patient needs.
Collaborative Care Model
The Collaborative Care Model (CoCM) is one of the most evidence-based approaches. In this setup, a primary care provider (PCP) leads the team but works alongside a care manager and a psychiatric consultant.
The care manager typically checks in with the patient regularly, offering counseling and tracking progress. If the patient isn’t improving, the psychiatric consultant reviews the case and advises the PCP on medication adjustments or new treatment strategies. The patient may never see the psychiatrist directly, but they benefit from their expertise through this coordinated team effort.
Integrated Primary Care
This model, often called the “Primary Care Behavioral Health” (PCBH) model, physically embeds behavioral health consultants (BHCs) within the primary care clinic.
When a doctor sees a patient with a behavioral need—whether it’s panic attacks, insomnia, or difficulty managing diabetes—they can introduce the patient to the BHC immediately. This is often called a “warm handoff.” The BHC provides brief, targeted interventions right in the exam room or a nearby office, functioning as a regular part of the primary care team.
Co-Located and Hybrid Models
Co-location simply means mental health and physical health providers share the same facility. While they might share a waiting room, they may not necessarily share the same medical records or treatment plans. However, physical proximity reduces the barrier to entry for patients.
Hybrid models are increasingly common, utilizing digital tools to bridge gaps. A clinic might have a nurse practitioner on-site, with a psychiatrist available via video link to consult on complex cases. This blend of physical and digital integration ensures that even small clinics can offer robust support.
Benefits of Integrating Mental Health into Healthcare
Moving toward a unified system offers profound advantages for both individual patients and public health as a whole.
Earlier identification and intervention is the most significant benefit. When mental health screenings are standard practice, conditions like depression or substance use can be caught in their early stages. Treating these issues early is far more effective—and less expensive—than waiting for a crisis.
Improved treatment outcomes follow naturally. When a patient receives care for both their diabetes and the depression that makes managing their diet difficult, both conditions improve. The coordinated approach ensures that one treatment doesn’t interfere with another.
Finally, integration helps reduce stigma. When a behavioral health consultant is just down the hall, seeing them feels as normal as seeing a nutritionist or getting an X-ray. It normalizes the experience of seeking help, reinforcing the idea that mental health is simply health.
Impact on Patients and Care Experience
For the average patient, the most immediate impact of integrated care is convenience. Navigating the U.S. healthcare system is notoriously difficult. Finding an in-network therapist, calling for availability, and traveling to a new office are significant hurdles.
Integrated care removes the friction. You go to your regular doctor—a place where you likely already feel comfortable—and get the help you need. This “whole-person” treatment approach makes patients feel seen and heard. It acknowledges that their headache might be stress-related or that their stomach issues could be tied to anxiety, rather than treating symptoms in isolation.
Role of Primary Care Providers
Primary Care Providers (PCPs) are the linchpin of integrated care. They are often the first, and sometimes the only, medical professionals a person sees.
In an integrated system, the role of the PCP expands. They are responsible for routine screening and referrals, using tools like the PHQ-9 (a depression questionnaire) as casually as a blood pressure cuff.
However, PCPs are not expected to be psychiatrists. Their role is to identify the need and manage the initial steps of ongoing mental health support, relying on their integrated team for specialized knowledge. This support structure prevents PCPs from burning out while trying to manage complex psychiatric needs on their own.
Technology Supporting Mental Health Integration
Technology has been a major accelerator for integration, especially in rural America.
Teletherapy and virtual care allow specialists to “beam in” to primary care offices. A patient in a rural clinic can sit in a private room and speak with a psychiatrist hundreds of miles away. This virtual integration expands the reach of the limited mental health workforce.
Behind the scenes, digital screening tools and EHR integration are vital. Electronic Health Records (EHR) that allow physical and mental health providers to see the same chart prevent dangerous drug interactions and ensure everyone is up to date on the patient’s status. Automated screening tools sent to patients’ phones before an appointment can also flag issues before the doctor even walks in the room.
Mental Health Integration and Chronic Disease Care
The link between chronic disease and mental health is undeniable. People with chronic conditions like heart disease, diabetes, and cancer are at a much higher risk for depression and anxiety. Conversely, untreated mental health issues can make it nearly impossible to manage a chronic illness.
For example, a patient with diabetes needs to manage diet, exercise, and medication daily. If that patient is also depressed, they may lack the motivation or energy to stick to that regimen. Integrated care addresses the depression alongside the diabetes. Coordinated treatment benefits the patient by creating a realistic care plan that accounts for their mental state, leading to better control of the chronic disease and a higher quality of life.
Workforce and Training Considerations
One of the biggest hurdles to widespread integration is the workforce. The U.S. is currently facing a severe shortage of behavioral health professionals. There simply aren’t enough psychiatrists and psychologists to staff every primary care clinic.
To bridge this gap, healthcare systems are focusing on cross-training clinicians. Nurses, physician assistants, and social workers are being trained in behavioral health basics. By empowering a wider range of staff to handle mild to moderate cases, the system reserves the highly specialized psychiatrists for the most complex patients.
Policy, Insurance, and Reimbursement Factors
Even with the best clinical models, integration cannot succeed without financial support. Historically, insurance companies reimbursed physical and mental health procedures differently, often paying less for the latter.
Coverage parity laws have attempted to fix this, legally requiring insurers to cover mental health services comparably to medical services. However, enforcement varies.
The shift toward value-based care incentives is helping. In this payment model, providers are paid based on patient health outcomes rather than the number of visits. Since untreated mental illness often leads to poor overall health and expensive hospitalizations, value-based care gives providers a financial incentive to integrate mental health services and keep patients healthier overall.
Challenges to Mental Health Integration
Despite the clear benefits, the road to full integration is paved with obstacles.
Funding and resource limitations are primary concerns. setting up an integrated practice requires upfront investment in hiring staff and updating facilities. For small, independent practices, this cost can be prohibitive.
Data sharing and privacy concerns also complicate matters. While HIPAA protects patient privacy, specific regulations regarding substance use records and mental health notes can make sharing data between providers legally complex. Systems must balance the need for seamless communication with the absolute necessity of protecting patient privacy.
Equity and Access in Integrated Care
Integration has the potential to be a great equalizer, but only if implemented thoughtfully. Underserved and rural populations stand to benefit the most, as they often have the least access to standalone mental health specialists. Bringing care into the local community clinic makes it accessible to those without the means to travel.
Cultural competency is equally important. Integrated care teams must be trained to understand how different cultures perceive mental health. In some communities, somatic symptoms (physical pain) are the primary way distress is expressed. Providers need to recognize these signs to offer effective, culturally sensitive care.
Is Mental Health Integration the Future of U.S. Healthcare?
The trajectory suggests that integrated care is not just a trend, but the future standard of medicine. System-wide adoption trends show major hospital networks and federally qualified health centers pivoting to this model.
Long-term sustainability will depend on continued policy support and payment reform. As data continues to prove that integrated care saves money by keeping people out of emergency rooms, insurance companies and government programs are likely to double down on their support. The future of U.S. healthcare looks less like a series of disconnected appointments and more like a unified team working toward total health.
FAQs – Mental Health Integration in the USA
What does mental health integration mean?
It means combining mental health care with primary medical care. Instead of going to separate offices, you receive support for both physical and behavioral needs in one setting, with doctors working together as a team.
How does integrated care improve outcomes?
By treating the whole person, doctors can address underlying issues that affect physical health, such as stress or depression. Coordinated care reduces medication errors and ensures patients follow through with treatment plans, leading to better overall health.
Is mental health integration covered by insurance?
Generally, yes. Most major insurance plans cover services provided in an integrated setting. Federal parity laws require mental health benefits to be comparable to medical benefits, though specific coverage can vary by plan.
What role does primary care play?
Primary care is often the entry point. Your general doctor screens for mental health issues, manages mild conditions, and coordinates with behavioral health specialists for more complex needs.
Will integrated care reduce stigma?
Yes. By treating mental health checks as a routine part of a standard doctor’s visit—just like checking blood pressure—it removes the fear and shame often associated with seeking help from a standalone psychiatric facility.
A Healthier Path Forward
The integration of mental health into the broader healthcare system represents a maturing of American medicine. It is an acknowledgment that we cannot treat the body while ignoring the mind. While challenges regarding funding and workforce remain, the momentum is undeniable. By breaking down the silos that have long separated our care, we are moving toward a system that is more accessible, more effective, and ultimately, more human.