Healthcare is one of the most critical aspects of any society, yet how it is delivered varies dramatically from one nation to another. If you have ever wondered why a doctor’s visit costs a small fortune in one country but is free at the point of service in another, the answer lies in the fundamental structure of their healthcare systems.
Understanding these differences is not just an academic exercise. It affects everything from how much tax you pay to how long you might wait for a surgery. While the United States often dominates headlines with its high costs and complex insurance networks, other nations have taken entirely different approaches. Some rely on government funding, others on strict mandates, and many use a blend of public and private options.
This article explores the nuances of global healthcare models, with a specific focus on how the US system stacks up against the rest of the world. We will break down the costs, access, and quality of care to provide a clear picture of what works, what doesn’t, and why these differences exist.
What Is a Healthcare System?
A healthcare system is the organization of people, institutions, and resources that deliver health care services to meet the health needs of target populations. At its core, it is the infrastructure that keeps a population healthy. This includes everything from hospitals and clinics to insurance companies, pharmaceutical manufacturers, and the government bodies that regulate them.
Key components of a healthcare system
Every functioning system relies on a few key pillars. First is the financing mechanism—how the money is raised and pooled to pay for services. This could be through taxation, private insurance premiums, or out-of-pocket payments. Second is the workforce: the doctors, nurses, and administrators who deliver care. Finally, there is the delivery of services, which covers primary care, specialized treatments, and emergency responses.
Why healthcare systems differ globally
No two countries have the exact same healthcare system meaning or structure because they are shaped by unique historical, political, and economic forces. A nation’s approach to healthcare often reflects its cultural values. For instance, countries that view healthcare as a fundamental human right tend to develop public, tax-funded systems. Nations that view it more as a service or commodity often lean toward private market solutions. Understanding healthcare systems globally requires recognizing that there is no single “correct” way to organize care; each model involves trade-offs between cost, access, and quality.
Major Types of Healthcare Systems Worldwide
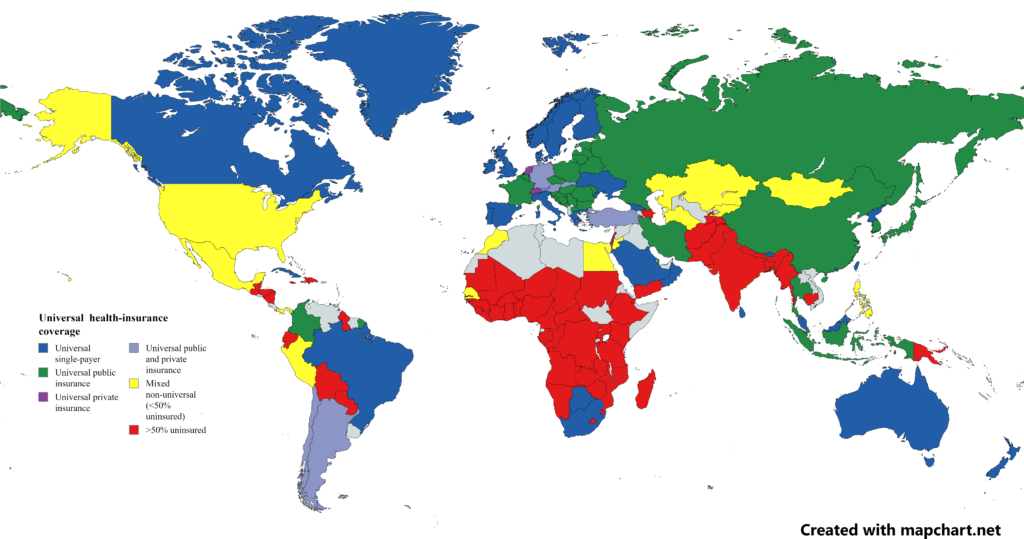
While every country tweaks the rules to fit its specific needs, most fall into one of four broad categories.
Public healthcare systems (The Beveridge Model)
In this model, healthcare is provided and financed by the government through tax payments. There are no medical bills at the point of service. Hospitals and clinics are often owned by the government, and doctors may be government employees. This is the system found in the United Kingdom (NHS), Spain, and New Zealand.
Private healthcare systems (The Out-of-Pocket Model)
This is common in less developed nations where there is no organized mass payment system. The rich get medical care; the poor stay sick or die. In these areas, patients must pay for their procedures out of their own pockets. If they cannot afford it, they do not receive care.
Universal healthcare models (The National Health Insurance Model)
This model uses private-sector providers, but payment comes from a government-run insurance program that every citizen pays into. Because there is no need for marketing, no financial motive to deny claims, and no profit, these universal insurance programs tend to be cheaper and much simpler administratively than American-style for-profit insurance. Canada, Taiwan, and South Korea use this system.
Hybrid healthcare systems (The Bismarck Model)
Used in Germany, Japan, and France, this system uses an insurance system usually financed jointly by employers and employees through payroll deduction. Unlike the US industry, these health insurance plans have to cover everybody, and they don’t make a profit. Doctors and hospitals tend to be private.
Understanding these types of healthcare systems helps clarify why global healthcare models produce such varied outcomes for patients.
How the US Healthcare System Works
The United States is unique among developed nations because it does not have a uniform healthcare system. Instead, it relies on a complex patchwork of public and private programs.
Role of private insurance
For many Americans, access to care is tied directly to private health insurance. These plans are sold by for-profit companies. They negotiate rates with healthcare providers and decide which services are covered. This market-based approach drives competition but also leads to significant administrative overhead and complexity for patients trying to navigate networks and deductibles.
Employer-sponsored healthcare
The backbone of the US healthcare system explained is employer-sponsored coverage. About half of the US population receives health insurance through their job. This arrangement dates back to World War II wage freezes, where companies offered benefits to attract workers. While it provides coverage for millions, it also ties health security to employment, meaning losing a job often means losing insurance.
Government programs and coverage gaps
The government fills in some gaps with programs like Medicare (for the elderly) and Medicaid (for low-income individuals). However, unlike other wealthy nations, the US does not guarantee universal coverage. Millions of people fall into coverage gaps—earning too much for Medicaid but not enough to afford private insurance. The healthcare system USA model remains the only one in the developed world that leaves a significant portion of its citizens uninsured or underinsured.
Healthcare Systems in Other Countries Compared to the USA
Comparing the US to its peers reveals stark differences in philosophy and execution.
Single-payer systems
Countries like Canada and the UK utilize single-payer systems. Here, the government acts as the sole insurer. This drastically reduces administrative costs because doctors don’t have to navigate hundreds of different insurance plans. It also gives the government immense leverage to negotiate lower prices for drugs and services.
Universal healthcare access
Almost all other developed nations operate under a mandate of universal access. Whether through government provision or mandatory non-profit insurance (like in Germany), the goal is ensuring that illness does not lead to financial ruin. In healthcare systems comparison studies, this universality is the primary differentiator between the US and the rest of the industrialized world.
Government-funded vs mixed models
While the UK is fully government-funded, countries like Australia use a mixed model. They have a robust public system available to everyone but encourage citizens to buy private insurance for faster access to elective surgeries. This USA vs global healthcare contrast highlights that “socialized medicine” isn’t the only alternative to the American model; many nations successfully blend public safety nets with private choice.
Cost of Healthcare: USA vs the World
The most glaring difference between the US and other nations is the sheer amount of money involved.
Healthcare spending per capita
The United States spends far more on healthcare than any other country. Healthcare costs USA vs world data consistently shows the US spending nearly twice as much per person as other wealthy nations like France or Canada. Despite this massive investment, US health outcomes are not consistently better, and in some metrics, they are worse.
Out-of-pocket costs
In systems like the UK’s NHS, out-of-pocket costs are negligible. In contrast, Americans often face high deductibles and co-pays even with insurance. Medical debt is a uniquely American problem among developed nations, standing as the leading cause of personal bankruptcy in the US.
Prescription drug pricing differences
Medical expenses comparison reveals that Americans pay significantly more for pharmaceuticals. Other governments negotiate drug prices directly with manufacturers, capping costs. The US market lacks this centralized bargaining power, allowing drug companies to set prices based on what the market will bear.
Access to Healthcare Services Globally
High costs might be justifiable if they guaranteed superior access, but the reality is mixed.
Wait times and appointment access
Critics of universal systems often point to long wait times. It is true that in countries like Canada, patients may wait longer for non-urgent elective procedures compared to insured Americans. However, healthcare access globally data suggests that for primary care and essential services, access is often better outside the US because cost is not a barrier.
Specialist care availability
The US excels in access to specialized care for those with good insurance. If you need a specific, complex procedure and have the means to pay, the US offers some of the fastest access to top-tier specialists. In contrast, healthcare wait times comparison studies show that patients in systems like the UK may face delays in seeing specialists for non-life-threatening conditions.
Emergency healthcare access
In emergencies, access is generally good across all developed nations. The difference lies in the aftermath. An ambulance ride and emergency surgery in France will not result in a bill. In the US, an out-of-network emergency can lead to financial distress, complicating the concept of true “access.”
Quality of Care and Health Outcomes
Does paying more result in better health? Not necessarily.
Life expectancy and mortality rates
Despite spending the most, the US has a lower life expectancy than comparable nations like Japan, Switzerland, and Australia. Infant mortality rates are also higher in the US. Global health outcomes data indicates that factors like obesity, opioid use, and unequal access to care drag down the US averages.
Preventive care effectiveness
Systems that prioritize primary care, like the Netherlands, excel at prevention. They manage chronic conditions effectively, keeping patients out of hospitals. The US system is often reactive, focusing on treating sickness rather than maintaining health. This approach drives up costs and can lead to lower healthcare quality comparison scores in areas like chronic disease management.
Patient satisfaction levels
Interestingly, patient satisfaction varies. Americans with high-quality insurance often report high satisfaction with their care quality. However, the general population in countries with universal systems often reports higher satisfaction regarding the security and affordability of their care, knowing they are covered regardless of life circumstances.
Advantages and Disadvantages of the US Healthcare System
To provide a balanced view, we must look at both the strengths and weaknesses of the American model.
Innovation and advanced treatments
The US is a global leader in medical innovation. The high prices paid for drugs and procedures help fund R&D for cutting-edge treatments. US healthcare pros and cons analysis shows that the country produces a significant portion of the world’s new medical technology and pharmaceuticals. Top US hospitals are consistently ranked among the best in the world for treating complex diseases like cancer.
Cost and affordability challenges
The primary disadvantage is cost. The system is inefficient, with high administrative overhead consuming nearly a quarter of healthcare spending. For the average citizen, the cost of premiums and deductibles has risen faster than wages, making healthcare a significant financial burden.
Coverage inequalities
The healthcare system USA analysis reveals deep inequalities. Quality of care is highly dependent on employment, income, and geography. While wealthy individuals receive world-class care, lower-income populations often face barriers that lead to poorer health outcomes.
Why Healthcare Systems Differ Across Countries
These differences aren’t accidental; they are the result of specific choices and circumstances.
Economic factors
Wealthier nations have more resources to dedicate to health. However, how they spend it matters. The US spends a huge percentage of its GDP on healthcare, while other efficient systems spend less for better coverage. Why healthcare systems differ often comes down to how efficiently a country can leverage its economic power.
Government policy and funding
Political will is a major driver. In many European nations, government policy focuses on social solidarity—the idea that society should collectively protect its members. This leads to funding models that redistribute costs.
Population health needs
Demographics play a role. Japan has an aging population, requiring a system focused on geriatric care and long-term management. Younger populations might prioritize maternal health and preventative services.
Cultural attitudes toward healthcare
Global health policy is deeply influenced by culture. If a culture prizes individualism (like the US), it may resist government mandates and prefer market solutions. Cultures that value collective welfare are more likely to support tax-funded, universal systems.
Common Myths About Global Healthcare Systems
Misinformation often clouds the debate around healthcare reform.
“Universal healthcare lowers quality”
This is a common global healthcare myth. Many countries with universal coverage, such as Switzerland and Germany, have health outcomes that equal or surpass the US. Quality is maintained through strict standards and competitive private provision within a public framework.
“Free healthcare means unlimited access”
“Free” at the point of service does not mean unlimited. Universal healthcare facts show that these systems rely on triage. You cannot necessarily demand an MRI for a minor headache instantly. Resources are allocated based on medical necessity, not ability to pay.
“The USA has the best healthcare system”
While the US has some of the best doctors and hospitals, having the “best system” implies that it works well for the entire population. Given the high costs and millions of uninsured, few comparative analyses rank the US system as the best overall.
Frequently Asked Questions (FAQ)
Does the USA have universal healthcare?
No, the United States does not have a universal healthcare system. It is a mixed public-private system where coverage depends on age, income, and employment status. While programs like Medicare and Medicaid cover specific groups, there is no guarantee of coverage for all citizens.
Why is healthcare more expensive in the USA?
Healthcare is more expensive due to higher prices for services and drugs (driven by a lack of central price negotiation), high administrative costs associated with private insurance, and the high salaries of medical professionals. The fee-for-service model also incentivizes more tests and procedures.
Which country has the best healthcare system?
Rankings vary by criteria. The Commonwealth Fund often ranks countries like Norway, the Netherlands, and Australia at the top due to their balance of access, equity, and health outcomes. No single country is perfect, but these nations consistently outperform others in comprehensive metrics.
Are wait times longer outside the USA?
For elective, non-emergency procedures, wait times can be longer in countries with national health systems like Canada or the UK. However, for emergency and primary care, wait times are often comparable or shorter than in the US, where financial barriers can also cause delays in seeking care.
Can the USA adopt another country’s healthcare model?
Adopting another model would be difficult due to the size of the US private insurance industry and political resistance to higher taxes or government control. However, the US could adopt specific elements, such as all-payer rate setting or public options, to improve its current hybrid system.
Final Thoughts on Global Healthcare System Differences
There is no perfect way to manage the health of a nation. Every model represents a choice between competing values: cost, speed, access, and equity. The US emphasizes choice and innovation but sacrifices universality and affordability. Other nations prioritize equal access and cost control but may limit provider choice or have longer waits for elective care.
Recognizing that healthcare systems differ globally allows us to look beyond national borders for solutions. We can appreciate the innovation of the US market while learning from the efficiency of German insurance or the equity of British public care. Ultimately, understanding these systems helps inform better policy discussions, moving us closer to a world where high-quality care is accessible to everyone.